

Main Phone: (520) 562-3321

At Gila River Health Care, we believe in team-based care that puts you at the center of your health journey.
Our Patient-Centered Care Team is here to support patients of all ages - children, teens, and adults - by working together to help you live your healthiest, happiest life.
Gila River Health Care has achieved certification as a Patient-Centered Care Team by the Joint Commission!

We have also received the American Indian Medical Home (AIMH) site designation from the Arizona Health Care Cost Containment System (AHCCCS), further enhancing our commitment to providing top-quality, culturally sensitive care.
How We Care For You:
Our approach focuses on you - your needs, values, and health goals. Here's what that means.
Click each one to learn more
We’re here for you with both appointment and walk-in options, along with dedicated phone support after hours.
We treat the whole person, respecting your needs, culture, and values.
We address both short-term and long-term health needs.
We help organize your care across different services, including specialists and community support programs.
We use trusted medical resources, track progress, and listen to patient feedback to provide the best care possible.
How We Support You:
- We aim to explain your plan of care in a way that's easy to understand so that you can make informed decisions about your health.
- We listen to your concerns and answer your questions.
- We refer you to specialists when necessary.
- We offer health education and tips to help you stay healthy.
- We help manage your health needs and connect you with the right services.
Your Role In Your Health Care:
- Schedule and attend appointments. Let your Care Team know in advance if you cannot make it.
- Share important health information including your medical history, symptoms and health goals.
- Keep us updated on any changes in your health.
- Bring a list of your medications to every visit.
- Follow your doctor's plan of care instructions.
Your Rights As A Patient:
We respect your rights as a patient and provide you with the opportunity to:
- Choose your clinicians within your Patient-Centered Care Team
- Seek a second opinion from a provider of your choice.
- Seek speciality care when needed.
Meet Your Care Team:
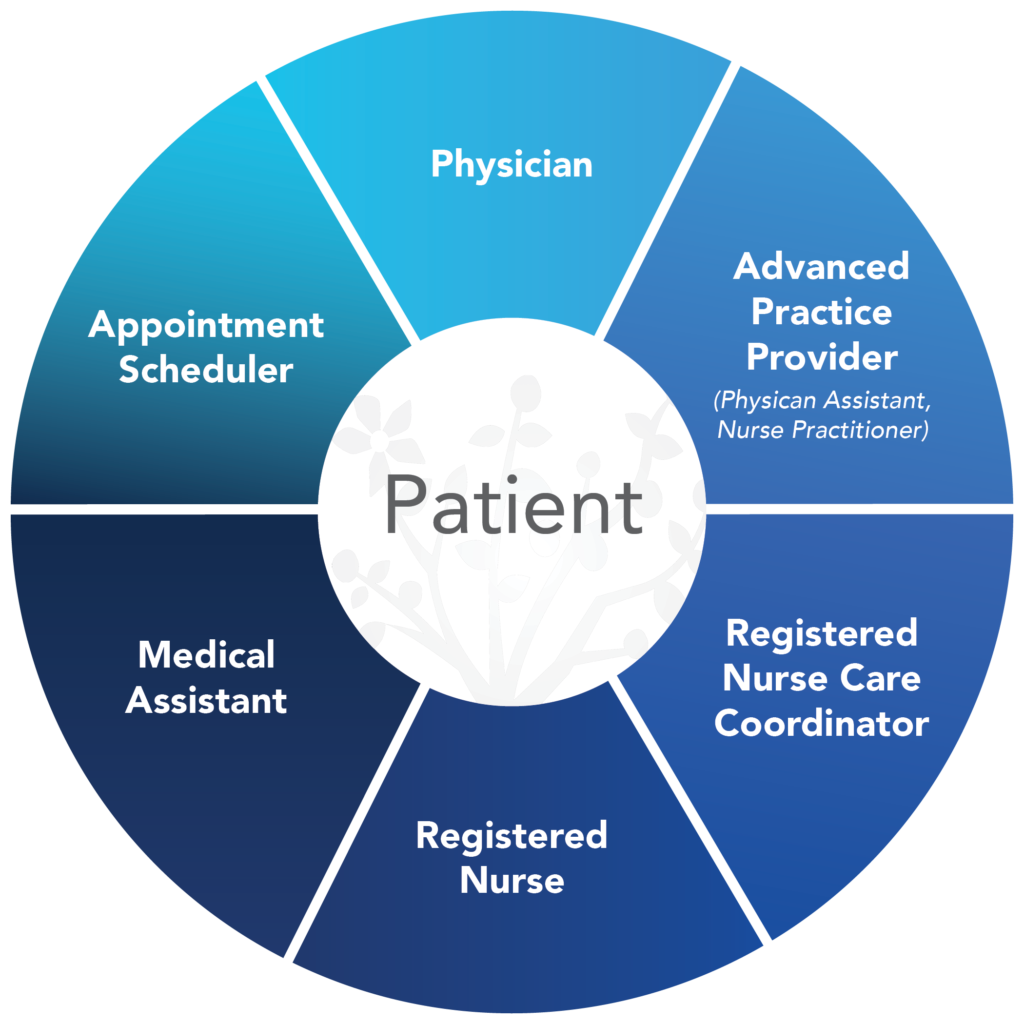
Click each location to meet our Patient-Centered Care Team
If you have any questions, please call our main phone (520) 562-3321


